More than half of the women in a new national survey were told by a healthcare provider that their symptoms were normal. They weren’t.
According to What They Didn’t Teach You in Sex Ed, a report released on April 20 by the reproductive health platform MyStoria, 54.3 percent of 1,000 female adults surveyed said they had been reassured by a provider, only to learn later that the reassurance was wrong. One in four said it had happened more than once. Nearly two-thirds needed more than one provider to get a meaningful answer to a reproductive health question. Another 9.2 percent gave up entirely.
That alone would be a bleak finding, but the more striking part came when MyStoria broke the data out by generation. Women in their late twenties, women in their thirties, early forties, and women in their late forties and early fifties reported the same gaps at statistically indistinguishable rates. Three age cohorts. One continuous story.
The timing is not coincidental. This week is Canadian Fertility Awareness Week and National Infertility Awareness Week in the United States, both running April 19 to 25. Below, we take a closer look at the survey, at MyStoria, and at why the company behind this research just made a strategic bet on the entire reproductive health lifecycle.
Who’s Behind the Survey: Meet MyStoria
MyStoria is a health technology platform based in Kitchener, Ontario, founded in 2024 by Jessica Chalk. The company describes itself, plainly, as “built for patients, by patients,” and its founder story is why that line lands differently than it usually does in health tech.
Chalk spent years inside the reproductive health system as a patient. She was diagnosed with endometriosis. She walked through an infertility journey that, in her own words, never ended the way she hoped. But the framing she returned to is not the diagnoses. It is the infrastructure that failed around her. Decisions made without her input. Treatments prescribed without explanation. Every wrong turn carrying an emotional and financial cost she was expected to absorb alone.
So she built the support layer she wished she’d had.
With a foundation in fertility care support, MyStoria is now built to support the full reproductive health lifecycle. Fertility, yes. But also painful periods, PCOS, endometriosis, perimenopause, and hormonal health. The iOS and Android apps launched with a freemium model, so the platform’s AI guidance and health record organization are free to start.
“Reproductive health has the highest dismissal rates, the longest diagnostic delays, and the most fragmented care of any condition. That is why we started here.”
Jessica Chalk, Founder and CEO, MyStoria
The Survey: Five Gaps Most Women Didn’t Know They Were In
MyStoria commissioned the survey of 1,000 female-identified adults in March 2026 through the Pollfish research platform. The female-only sample was, in the company’s words, “an intentional design decision reflecting the disproportionate navigational burden reproductive health places on women, including in couples-based and male-factor fertility situations.”
The report identifies five interconnected gaps that compound over a lifetime of reproductive health decisions: knowledge, dismissal, generation, navigation, and tools. The numbers behind each one are worth sitting with.
Knowledge. 56.0 percent of respondents said school-based sex education did not prepare them for adult reproductive health. Only 22.8 percent agreed that it did.
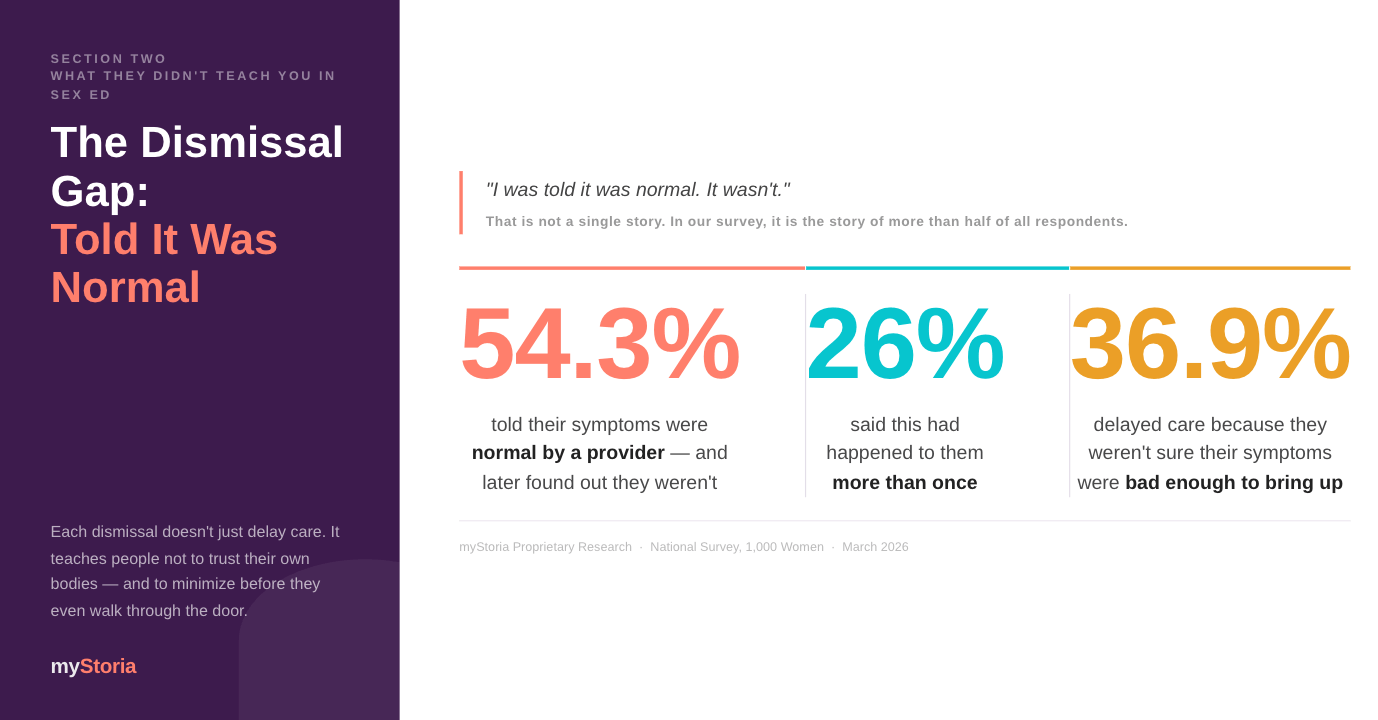
Dismissal. 54.3 percent were told their symptoms were normal by a healthcare provider, only to later learn that they weren’t. One in four said this had happened more than once.
Navigation. 62.8 percent needed more than one provider to get a meaningful answer to a reproductive health question. Another 9.2 percent gave up entirely. Another 9 percent said they were still looking.
Delay. 36.9 percent delayed care because they weren’t sure their symptoms were bad enough to bring up. It was the single most common barrier to care, cited more often than wait times, cost, embarrassment, or not knowing the right provider.
Life stage. 41.6 percent first learned about perimenopause and menopause only after symptoms had already started, making it the most commonly cited condition in the survey.
The pattern that emerges is not individual patients missing appointments, or individual doctors missing diagnoses. It is a system in which the average person enters reproductive health care underprepared, is disbelieved when they try to describe what is happening, is bounced between providers to assemble an answer, and learns about the next life stage only once it is already underway.
Research outside the survey supports the direction of every finding. Endometriosis alone takes an average of almost seven years to diagnose, with some regional studies reporting an average of 10 years. For PCOS, roughly one-third of women report more than two years to diagnosis, and close to half consult three or more health professionals before they get one. And 80 percent of graduating internal medicine residents report not feeling competent to discuss or treat menopause. The MyStoria survey describes, in one sample, what clinicians have been documenting in pieces for years.
The Gap That Didn’t Close
The most arresting finding in the report is what did not change across the three age cohorts MyStoria analyzed: respondents in their late twenties, those in their thirties and early forties, and those in their late forties and early fifties.
Between 41 and 44 percent of respondents across all three cohorts first learned about a reproductive health condition only after symptoms had begun. Between 52 and 59 percent said sex education had not prepared them for adult reproductive health. Between 34 and 38 percent had delayed care because they weren’t sure their symptoms warranted attention.
Three generations. Statistically identical gaps.
“This is not a story about individual providers failing individual patients. It is a story about a system that was never designed to prepare us for our own bodies. The data confirmed what we built MyStoria to address: most people enter the reproductive health system without the information they need to use it well, and the system does not fill that gap.”
Jessica Chalk, Founder and CEO, MyStoria
The quiet implication is that the interventions that should have reached women in their forties didn’t. Neither did the ones that should have reached their daughters. Neither did the ones aimed at the generation after them. That is what a system-level problem looks like when you put three decades of it in a single chart.
It also reframes a familiar exchange. When a woman in her thirties says, “I wish I’d known,” she usually hears back, “Well, you know now.” The MyStoria data suggests the truer answer is: your mother said the same thing. So will your daughter, unless something changes.
What People Actually Wanted
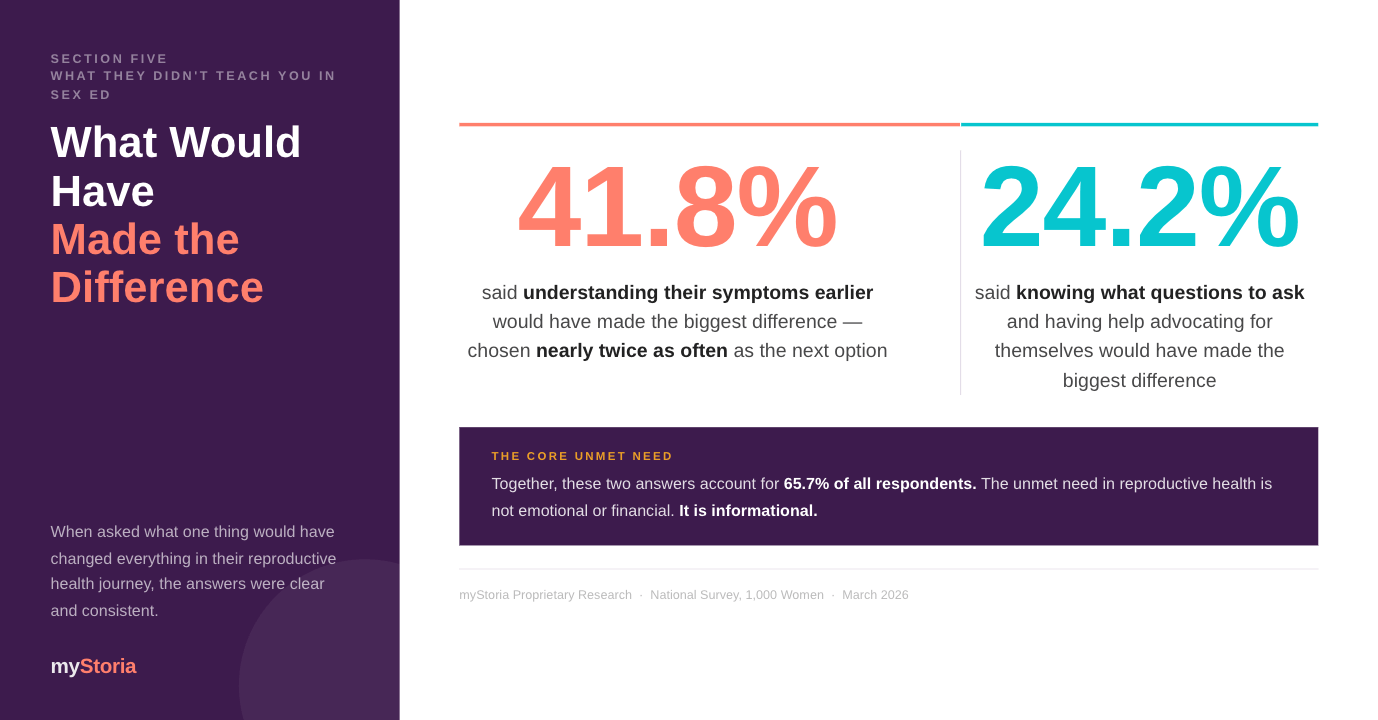
When respondents were asked which single thing would have made the biggest difference on their reproductive health journey, 41.8 percent said understanding their symptoms earlier. A further 24.2 percent said knowing what questions to ask and how to advocate for themselves. Together, those two answers account for 65.7 percent of all respondents.
“The data makes clear the need is not primarily financial or emotional. It is informational.” That is how the report itself puts it.
This is a meaningful reframe. In most conversations about reproductive health access, cost and emotional toll get the most airtime, for good reason. But the women in this sample described something quieter and older: they did not have the words, and the people who did weren’t sharing them.
The time burden is also significant. Nearly one in three respondents (29.5 percent) said they spend one to three hours per week on reproductive health management tasks: researching, booking, following up on referrals, tracking symptoms, coordinating between providers. That labor falls almost entirely on the patient.
If you’ve spent time in any fertility or chronic-condition community, none of this is news. What is new is seeing it quantified in a nationally representative sample, across three generations, at the same time.
Why This Week
It is not an accident that the report landed on April 20. That is the opening day of Canadian Fertility Awareness Week and National Infertility Awareness Week in the United States, both running April 19 to 25, 2026. NIAW’s theme this year is, fittingly, “More Than.”
Awareness weeks are sometimes treated as ceremonial. This one has teeth. Canada’s Fertility Matters organization uses the week to push for provincial funding and public education. RESOLVE, which founded NIAW in 1989, treats it as its annual advocacy surge with Congress. Both fall squarely inside the space the MyStoria survey is describing: the gap between what women are told about reproductive health and what they actually need to navigate it.
Which is to say: the survey isn’t just data. It is a contribution to an advocacy conversation that was already happening this week, and a challenge to anyone who still thinks awareness is enough on its own.
What to Do With This Information
If you are reading this and recognizing yourself in the numbers, a few things are worth doing.
1. Write your own history down, in one place. MyStoria is one option, and its free tier is built exactly for this. But even a plain document or a note on your phone listing your symptoms, cycle patterns, test results, and previous providers’ advice is worth more than you think. “I carry years of history in my head” is one of the most common things patients tell Chalk’s team, and the fix is mechanical: get it out of your head.
2. Name dismissal when it happens. One phrase most clinicians respond to is, “I’d like this documented in my chart.” If a provider tells you something is normal and you disagree, that sentence changes the conversation. It also leaves a paper trail you can bring to your next appointment.
3. Ask specifically what “normal” means. When a test result or symptom is labeled normal, ask: normal for whom, at what age, and on which criteria? The American College of Obstetricians and Gynecologists publishes plain-language patient education on most major reproductive health topics, and it is a fair starting point for your own benchmarking.
4. Front-load learning about the next life stage. 41.6 percent of women in the MyStoria survey first learned about perimenopause after symptoms started. You do not have to. ACOG and the Mayo Clinic both maintain free, patient-facing overviews, and books and podcasts on perimenopause have multiplied in the last two years. The current knowledge base is imperfect, but it is meaningfully better than what was available to the cohort ahead of you.
5. Treat your providers as consultants, not authorities. The women who got answers, per the MyStoria data, were the ones willing to seek a second (or fourth) opinion. That is not a character trait. It is a survival skill in a system that, by its own admission, struggles to diagnose the conditions most women will navigate.
The Layer That Was Missing
Reproductive health, as Chalk puts it, is one of the most personal journeys a person can face. It is also one of the most under-supported. The MyStoria survey is a quantitative portrait of exactly how under-supported, across a longer stretch of time than most of us realize.
That is the harder news. The better news is that this is no longer a problem the healthcare system is being asked to solve alone. A new generation of companies, MyStoria among them, is starting from the premise that the patient should not have to be her own care coordinator, medical historian, and insurance analyst while also being the person whose body is the subject of the appointment. Whether this approach becomes the standard will depend, in part, on whether the data keeps pushing in the direction this survey does.
The gap did not close on its own. It is starting to close because people decided to build over it.
Resources
What They Didn’t Teach You in Sex Ed (Full MyStoria Report): The full research report released April 20, 2026, with all findings and methodology.
MyStoria Press Release: The official release covering the survey’s key findings and founder commentary.
MyStoria Seed Round and Lifecycle Expansion: Details on the $1.625M seed round and the platform’s move beyond fertility.
Canadian Fertility Awareness Week: Fertility Matters Canada’s annual awareness and advocacy week.
National Infertility Awareness Week: RESOLVE’s U.S. awareness week, running April 19 to 25, 2026. 2026 theme: More Than.
ACOG Menopause Resource Hub: Free, patient-facing education on perimenopause and menopause.

